The Alarming Truth About 4 Stages of Appendicitis
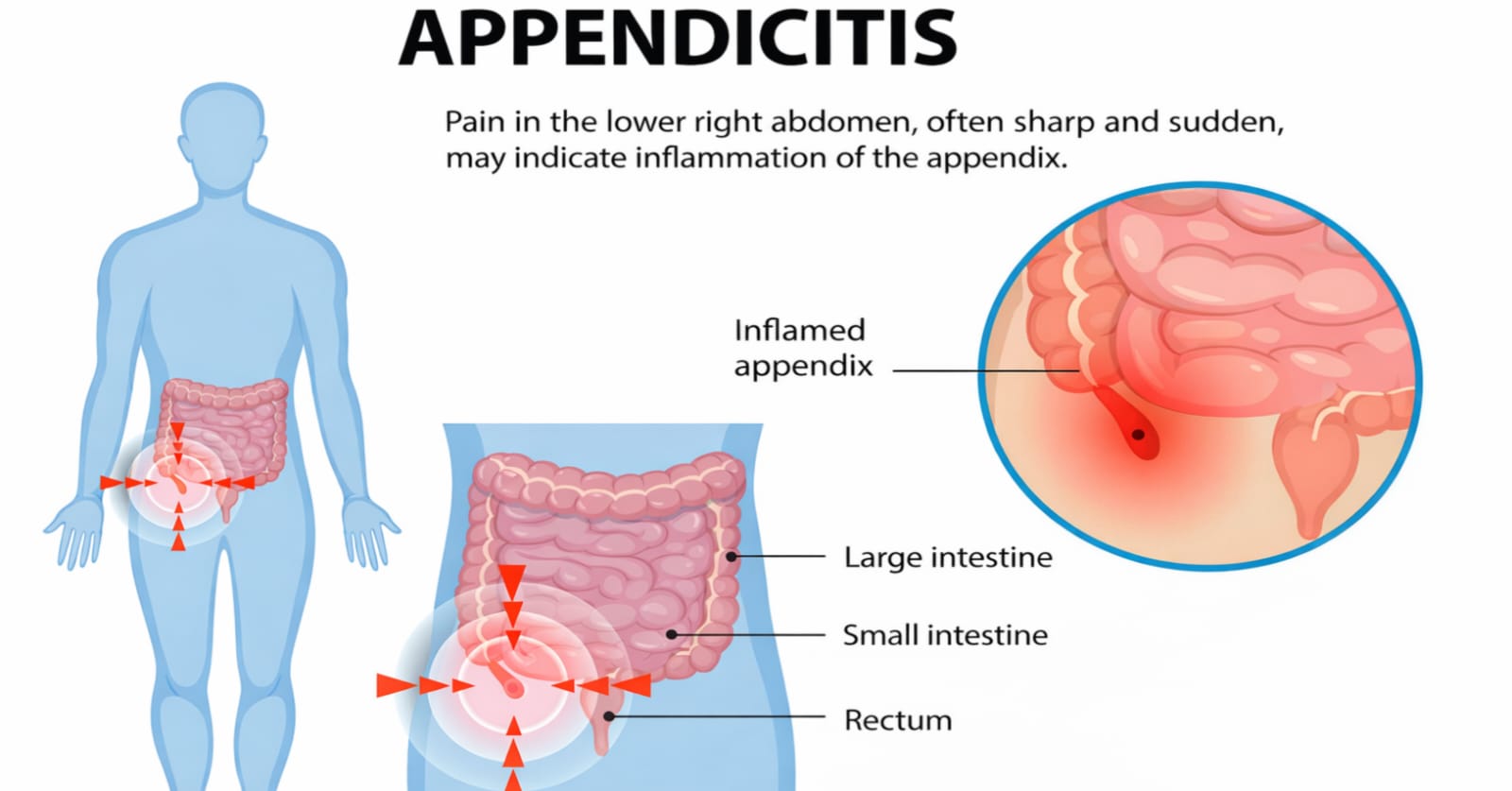
Appendicitis is a condition that occurs when the appendix becomes inflamed, swollen, and infected. The appendix is a small, finger-shaped pouch attached to the large intestine on the lower right side of the abdomen. Although it does not have a vital function in modern human digestion, inflammation in this small organ can quickly become dangerous if ignored. Many people underestimate stomach pain, but this particular condition can progress rapidly and lead to serious complications.
The reason this illness demands attention is its unpredictable nature. It often begins with mild discomfort that feels similar to common digestive issues. Within hours or days, however, that discomfort can transform into severe pain requiring emergency surgery. Because symptoms can overlap with other abdominal problems, early recognition is extremely important.
Understanding how the condition progresses through different stages helps people recognize warning signs sooner. Medical professionals typically describe four stages, each representing increasing severity. Knowing these stages can make the difference between simple treatment and life-threatening complications.
Stage One: Early Inflammatory Phase
The first stage begins when the inner lining of the appendix becomes irritated and inflamed. This irritation is often caused by a blockage inside the organ. The blockage may result from hardened stool, swollen lymph tissue, or infection. At this early point, swelling is mild, and blood flow is still largely intact.
Symptoms during this phase are often subtle. A person may feel vague discomfort around the belly button area, mild nausea, or a slight loss of appetite. The pain is usually dull rather than sharp, which makes it easy to dismiss. Some individuals may experience a low-grade fever, but it may not seem serious.
If diagnosed during this stage, treatment outcomes are generally excellent. Surgical removal of the appendix is straightforward, and recovery is typically quick. The challenge is that many people delay seeking help because the pain feels manageable at first. Early medical evaluation is the safest approach whenever abdominal pain persists or worsens.
Stage Two: Suppurative Phase
As inflammation continues, the condition moves into the suppurative stage. During this phase, pus begins to accumulate inside the appendix. The swelling increases, and pressure builds within the organ. Blood flow becomes more restricted, and the infection intensifies.
The pain now shifts from the center of the abdomen to the lower right side. It becomes sharper and more localized. Walking, coughing, or even slight movement may worsen the discomfort. Fever becomes more noticeable, and vomiting or loss of appetite is common. At this point, most individuals realize that something is seriously wrong.
Medical intervention during this stage is urgent but still manageable. Surgery is usually required, and antibiotics may be administered to control infection. Prompt treatment prevents further damage and significantly reduces the risk of complications. Delay, however, allows the condition to progress to far more dangerous stages.
Stage Three: Gangrenous Phase
If the infection continues untreated, blood supply to the appendix can become severely compromised. When tissue does not receive enough oxygen and nutrients, it begins to die. This stage is known as the gangrenous phase, and it marks a dramatic escalation in severity.
Pain during this stage often becomes intense and constant. The abdomen may feel rigid, and touching the area can cause significant discomfort. Fever may rise higher, and a person might feel weak, fatigued, or confused. The immune system struggles to contain the spreading infection, which increases the risk of rupture.
Surgery during this stage is more complex than in earlier phases. The surgeon must remove the damaged tissue and carefully clean the surrounding area to prevent infection from spreading. Recovery may take longer, and hospital stays are often extended. Quick action is critical to avoid life-threatening consequences.
Stage Four: Perforated or Ruptured Phase
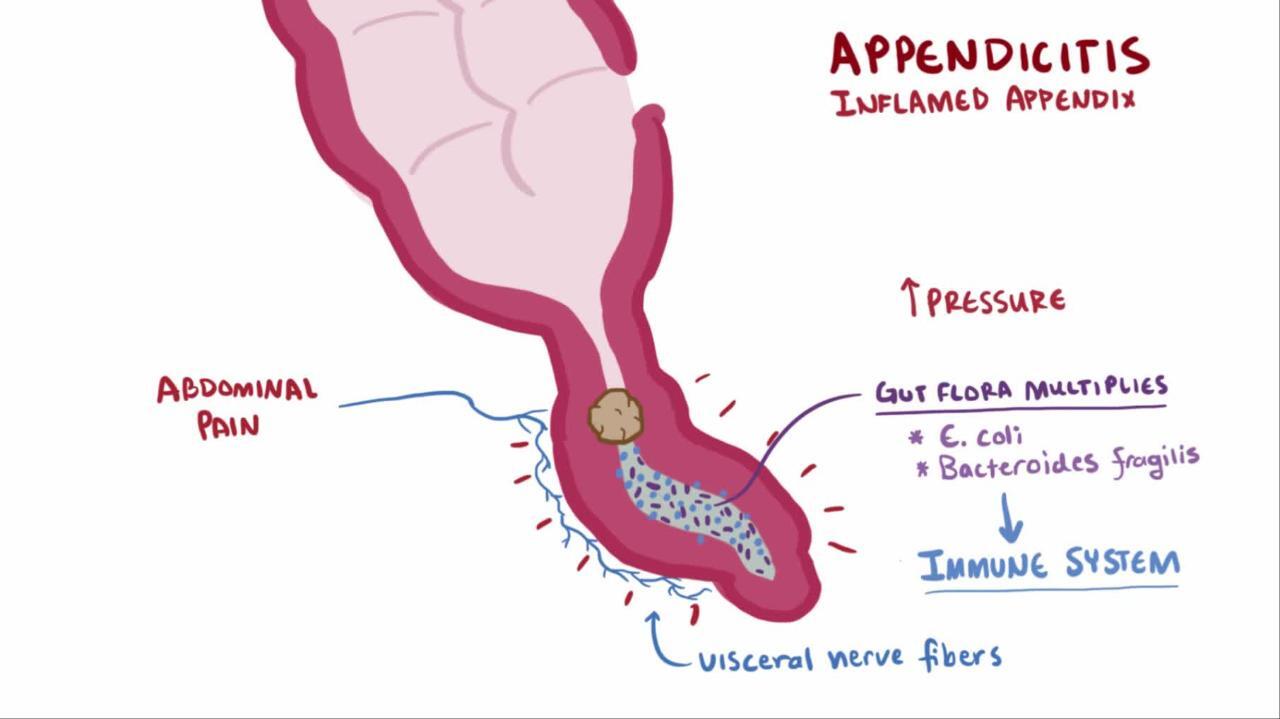
The most severe stage occurs when the appendix bursts. Once it ruptures, infected material spills into the abdominal cavity. This leads to a serious condition called peritonitis, which is an inflammation of the abdominal lining. At this point, the infection is no longer confined to one small organ.
Interestingly, some individuals notice a brief decrease in pain right after rupture because internal pressure is relieved. However, this relief is short-lived. Soon after, severe and widespread abdominal pain develops. High fever, chills, rapid heartbeat, and extreme weakness can follow. Immediate emergency care is essential.
Treatment at this stage involves urgent surgery and strong intravenous antibiotics. Doctors must remove the appendix and clean the abdominal cavity thoroughly. Hospitalization is longer, and complications such as abscess formation may occur. This stage highlights why early recognition and prompt care are so important.
Key Differences Between the Four Stages
Understanding how the stages differ helps clarify why timing plays such a critical role. The table below summarizes the progression from mild inflammation to rupture and shows how symptoms intensify over time.
| Stage | Main Internal Change | Pain Location | Severity Level | Urgency of Treatment |
|---|---|---|---|---|
| Early Inflammatory | Mild swelling and irritation | Around belly button | Mild to moderate | Urgent but stable |
| Suppurative | Pus formation and increased pressure | Lower right abdomen | Moderate to severe | Immediate medical care |
| Gangrenous | Tissue death due to reduced blood flow | Intense lower right pain | Severe | Emergency surgery |
| Perforated | Rupture and spread of infection | Widespread abdominal pain | Critical | Life-threatening emergency |
This progression shows how rapidly inflammation can escalate. What begins as manageable discomfort can transform into a medical crisis within a short period. Recognizing changes in pain location and intensity is often the key to early diagnosis.
While not every case follows an identical timeline, the overall pattern remains consistent. Early intervention dramatically reduces risks, shortens recovery time, and prevents dangerous complications. Awareness empowers individuals to act before serious damage occurs.
Causes, Risk Factors, and Prevention Insights
Although the exact trigger is not always clear, blockage inside the appendix is the most common cause of inflammation. Hardened stool, infection, or swelling of nearby lymph tissue can obstruct the narrow opening. Once blocked, bacteria multiply quickly, leading to swelling and infection.
Certain groups may face slightly higher risk, including teenagers and young adults. However, the condition can occur at any age. A diet low in fiber may contribute to constipation, which in turn increases the likelihood of blockage. Family history can also play a minor role, though it is not a direct cause.
There is no guaranteed way to prevent this condition entirely. However, maintaining a balanced diet rich in fruits, vegetables, and whole grains may support digestive health. Paying attention to persistent abdominal pain and seeking early medical advice remains the most effective strategy for avoiding serious outcomes.
Diagnosis and Treatment Approaches
Doctors rely on a combination of physical examination, medical history, and imaging tests to confirm inflammation of the appendix. Pressing on the lower right abdomen often reveals tenderness. Blood tests may show elevated white blood cells, indicating infection. Imaging techniques such as ultrasound or CT scans provide a clearer picture.
Treatment typically involves surgical removal of the appendix, a procedure known as an appendectomy. This surgery can be performed through traditional open surgery or minimally invasive laparoscopic methods. In some early cases, antibiotics may be used initially, but surgery remains the most definitive treatment.
Recovery time varies depending on the stage at diagnosis. Early-stage cases often allow patients to return home within a day or two. More advanced cases may require longer hospital stays and extended recovery periods. Following medical advice carefully ensures proper healing and reduces the risk of complications.
Conclusion
Appendicitis may begin quietly, but it can escalate with alarming speed. From mild inflammation to rupture, the four stages demonstrate how quickly a small organ can create a serious health emergency. Recognizing the shift from vague discomfort to sharp lower abdominal pain is one of the most important warning signs.
Early medical attention is the single most effective way to prevent complications. While surgery may sound frightening, timely treatment is safe, common, and highly successful. Delaying care, on the other hand, increases the risk of infection spreading throughout the abdomen.
Understanding these stages empowers individuals to act decisively. Persistent or worsening abdominal pain should never be ignored. When addressed promptly, this condition is treatable, recovery is smooth, and long-term health can be preserved.
FAQs
How quickly can appendicitis progress through its stages?
It can progress within 24 to 72 hours, though the timeline varies. Some cases move faster than others, which is why early evaluation is important.
Can appendicitis go away on its own?
In rare situations symptoms may temporarily improve, but the underlying issue usually requires medical treatment. Ignoring it increases the risk of rupture.
Is surgery always necessary?
Surgery is the standard treatment. In selected early cases, doctors may try antibiotics first, but recurrence is possible.
What does appendicitis pain feel like?
It often starts as dull pain near the belly button and later becomes sharp pain in the lower right abdomen. Movement usually worsens it.
How long does recovery take after surgery?
Most people recover within a few weeks. Early-stage cases heal faster, while advanced stages may require longer rest and monitoring.